
Harm Reduction Saves Lives
DOWNLOADAugust 5, 2022 - Lauren Kennedy, Tanner Derror and Elizabeth Williams, Michigan State University Extension
Steps for Responding to an Opioid Overdose
If someone is overdosing, their breathing may be very slow or erratic or they may not be breathing at all. They cannot be awakened. Their heart rate will be very slow or may have stopped. Their skin may be blue-gray or pale as well as clammy. Their fingernails or lips may be blue or purple. Their pupils will be tiny pinpoints. You may hear them snoring or you may hear deep gurgling or choking noises.
Follow these steps:
- Try to wake the person up. Shake them, shout that you’re calling 911, say their name if you know it, and pinch the skin on their upper arm. You can also try pinching their ear lobe, back of the neck, or Achilles heel to wake them up.
- Use naloxone/Narcan if you have it. Follow the directions for the type of naloxone you have (spray or injection). Some opioids may have higher potency, so you can administer a dose of naloxone every 2 minutes while you wait for emergency personnel to arrive.
- Call 911. Tell them that the person is unresponsive and not breathing. You do not need to mention a possible overdose; just stick to the facts that the person is unresponsive and/or not breathing.
- Provide rescue breathing if you know how. Lay them on their back, and tilt their head back. Pinch their nose and put your mouth over theirs to form a seal. Give a breath every 5 seconds. If their chest (not their stomach) begins to rise and fall, it is working.
- If the person begins to breathe regularly on their own, put them into the recovery position (see picture below for more details on the recovery position). If they do not begin to breathe regularly on their own, follow the instructions of the 911 operator or perform rescue breathing, if you know how.
It is important to stay with someone once they regain consciousness. They may be dopesick from the effects of naloxone or they may have used long-acting opioids, and will need continued help and care. Sometimes an overdose is not the only health condition a person is experiencing at that time, so they will likely need medical care once they’re conscious. Also, re-overdoses are possible, so make sure the person doesn’t use drugs again until the initial naloxone dose(s) wear(s) off.
Michigan’s Good Samaritan Law: What You Should Know
Michigan’s Good Samaritan Law (Public Act No. 307 of 2016) does include some protections for people using drugs to avoid arrest or prosecution for possession or use.
- According to the law, if you seek medical care (for example, calling 911, reporting a medical emergency to law enforcement and other situations.) or are incapacitated and presented for medical care by someone else, you are exempt from arrest and prosecution of possession or use of a controlled substance, but only if the amount you possessed was sufficient only for personal use. Personal use amounts can vary according to the type of substance.
- If you are presenting someone for medical assistance, you are only exempt from prosecution or arrest if the evidence was obtained as a result of seeking medical assistance or accompanying another individual who requires medical assistance to a facility or agency.
Michigan’s Good Samaritan Law does not protect people from arrest for any other criminal offenses, such as selling drugs, driving while drugged, sex work, or possession of banned substances in larger amounts than personal use.
Protections under the law are not always applied uniformly and people who use drugs may feel some understandable reluctance to involve police and medical providers. However, it is better to do something to help, to do anything you can safely manage, than to do nothing to help someone experiencing an opioid overdose. If calling 911 is not an option for you, try to find someone nearby who can call instead. Administer naloxone, attempt rescue breathing, put the person in the recovery position, and alert someone to the emergency so they can step in and help.
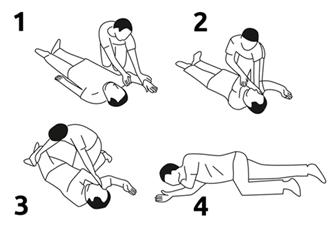
Recovery Position
- Kneel beside the person. Stretch the arm closest to you out from their body.
- Fold the other arm over their chest.
- Bend their leg at the knee.
- Gently roll the person on to their side, supporting their head and neck. Tilt their head back and make sure their airway is clear.
Harm reduction is a set of evidence-based, practical strategies and tools that reduce the potential harmful consequences that result from drug use. Harm reduction is judgment free. It respects the human rights of all people, including people who use drugs. It saves lives.
Harm reduction for people who use drugs includes the following examples:
- Naloxone/Narcan
- Drug checking supplies (for example, fentanyl test strips)
- Sterile pipes and smoking kits
- Sterile syringes and needles
- Safe consumption sites
- Personal care and hygiene items (lip balm, bandages, and other items)
- Medical referrals and testing
Supporting harm reduction strategies in your community increases the likelihood that people will receive the care they need to stay alive.
Contact your local health department or reach out to a Michigan State University Extension educator in your county if you would like more information on receiving harm reduction information or supplies.
Want to explore local options for substance use disorder treatment, family support, and harm reduction? Visit our collection of local, state, and national resource guides.
You are loved.
References and Resources
National Harm Reduction Coalition. (n.d.) Opioid overdose basics: Responding to opioid overdose. https://harmreduction.org/issues/overdose-prevention/overview/overdose-basics/responding-to-opioid-overdose/
Substance Abuse and Mental Health Services Administration. (2018). SAMHSA opioid overdose prevention toolkit (Rev. ed.) (HHS Publication No. [SMA] 18-4742). U.S. Department of Health and Human Services. https://store.samhsa.gov/sites/default/files/d7/priv/sma18-4742.pdf
Substance Abuse and Mental Health Services Administration. (2022). Opioid overdose. U.S. Department of Health and Human Services. https://www.samhsa.gov/medication-assisted-treatment/medications-counseling-related-conditions/opioid-overdose



 Print
Print Email
Email







