Research attacks allergic airway disease in its infancy
Michigan State University (MSU) AgBioResearch scientist James G. Wagner has been applying knowledge in airway toxicology to study the effect that air pollution and toxins have on lung function -- specifically the incidence of asthma.
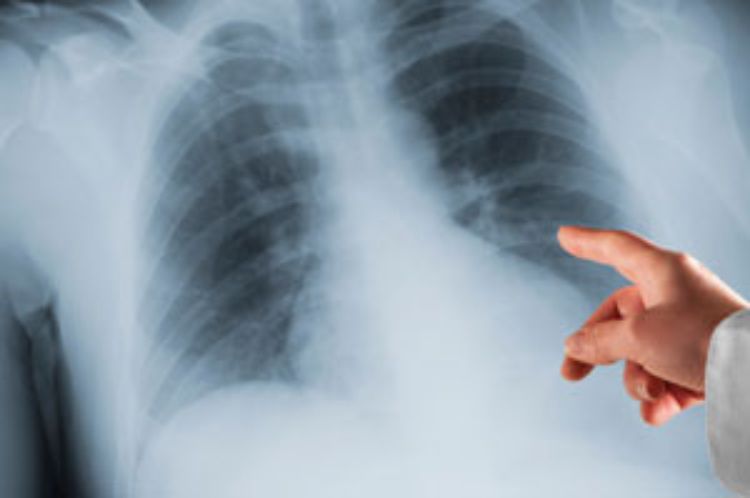
Asthma rates in the United States have more than doubled in the past 30 years. It is estimated that chronic respiratory disease afflicts more than 8 percent of the population (24.6 million) today compared with 3 percent in 1980. The highest prevalence — nearly one in 10 — is recorded in children (ages 0–17), according to the 2009 National Health Statistics Report.
Michigan State University (MSU) AgBioResearch scientist James G. Wagner, associate professor in the Department of Pathobiology and Diagnostic Investigation, has been applying knowledge in airway toxicology to study the effect that air pollution and toxins have on lung function -- specifically the incidence of asthma. Some of his recent work focuses on a lesser known form of vitamin E called gamma-tocopheral (γT) and its potential to alleviate allergic airway disease.
“The vitamin E that most people are familiar with is alphatocopheral (αT), which is found in multi-vitamin supplements, and its consumption is encouraged for its antioxidant capacity among other benefits,” Wagner said. “But our research focused on γT, another form of vitamin E. We found in the rodent model that γT can protect from and reverse allergic inflammatory processes of the lung. We suspect it does so by inhibiting the enzyme cyclooxygenase-2 [COX2], which is a key inflammatory pathway.”
One of eight forms of vitamin E, γT is found in such foods as corn and soybean oils, red and green peppers, walnuts, oregano and chestnuts. It has been shown to protect against nitrogen-based free radicals, which play an important role in diseases associated with chronic inflammation, including cancer, heart disease and degenerative brain disorders such as Alzheimer’s disease.
Wagner is also exploring a possible connection between γT consumption during pregnancy and the incidence of allergic airway disease in children. He has partnered with pediatric respiratory physician Graham Devereux, of Royal Aberdeen Children’s Hospital in Aberdeen, Scotland.
“One of Devereux’s initial findings showed that women who had low vitamin E intake had children with more wheeze or allergy airway symptoms at ages 2 and 5,” Wagner said. “I asked if that was γT or αT and he wasn’t sure, so I suggested we find out together.’”
They tested three groups of pregnant mice receiving the following doses of vitamin E (αT form): recommended intake, less than 50 percent of recommended intake, and four times the recommended daily amount.
“We found that the pregnant mice with deficient vitamin E had more pups with worse asthma,” said Wagner, who presented the data at the 2011 International Meeting of the American Thoracic Society. “But we also found that giving mice extra vitamin E really didn’t help at all. So it appears to be more of an issue with deficiency.”
On the basis of preliminary findings, Wagner believes setting a recommended daily amount (RDA) of γT might be beneficial. And although many pregnant women in the United States take a multi-vitamin, Wagner said the vitamin E form in a multi-vitamin is αT, not γT. He said that γT is one of the vitamin E forms that have been relatively ignored over the years.
In addition, results from his continuing studies show that the superiority of γT over αT to limit allergic airway symptoms is also evident in adult mice.
“You can start supplementing diets with tocopheral in adult mice and see the effect of γT. You do not have to start in utero,” Wagner said. “Our hypothesis is that γT may have a role in appropriate immune cell development in utero and in growing children.”
Wagner’s research with vitamin E is ongoing.
“There are six other isoforms [in addition to γT and αT] that are just now being studied and appreciated more. Some of them are called tocotrienols and have been shown to have anti-inflammatory properties, at least in the Petri dish.”
Wagner is already working with AgBioResearch scientist Norm Hord, associate professor in the MSU Department of Food Science and Human Nutrition, to look at whether consuming foods containing high levels of αT and γT has the same impact on allergic airway disease as the supplements do.
“Usually when we mix food for rodents in the lab, we combine powders with corn oil,” he said. “In this instance, we substituted the corn oil with walnut oil that contains high γT, and we used almond oil that contains high αT. The animals fed the walnut oil diet had better lung function than the others.”
One challenge with this particular study is determining whether people can consume enough γT through normal dietary intake, Wagner said.
“Some researchers believe that your body will more easily absorb the vitamins in a natural state, such as in food, as opposed to a supplement,” he said. “I’m not so sure I believe that. Not yet anyways.”



 Print
Print Email
Email




